Overdoses Tripled in New Jersey Despite Limits on Rx Opioids
By Pat Anson, PNN Editor
September 3, 2021
In 2017, New Jersey became one of the first states in the country to impose a hard limit on initial opioid prescriptions, with patients allowed only a 5-day supply of opioid pain medication. If they needed more, their doctor would have to write a new prescription, enroll patients in a pain management program, and counsel them about the risks of opioid addiction and overdose.
“We are here today to save lives,” then-Governor Chris Christie said after signing the legislation into law. “New Jersey now leads the way first and foremost in recognizing this is a disease.”
Four years later, there is little evidence the 5-day limit has reduced opioid addiction or saved lives in New Jersey. In fact, it may have made the overdose crisis worse by forcing some patients to turn to increasingly dangerous street drugs.
A new study at Rutgers University, recently published in The Journal of Substance Abuse Treatment, found that medically treated opioid overdoses among Medicaid patients more than tripled in New Jersey from 2014 to 2019.
Researchers found the overdose rate continued to rise even after the 5-day opioid limit was imposed, with opioid prescription rates nearly cut in half for Medicaid beneficiaries, falling from 23 percent in 2015 to 13 percent in 2019.
The rising number of overdoses was primarily due to heroin and illicit fentanyl, and often involved alcohol and other drugs. Medicaid patients suffering from alcoholism, benzodiazepine addiction, depression, hepatitis C, heart failure and pneumonia had overdose rates at least 1.5 times higher than other beneficiaries.
“While high rates of opioid prescribing likely contributed to earlier increases in OUD (opioid use disorder), actions to further limit such prescribing alone may do little to reduce opioid overdose in the current environment,” wrote lead author Stephen Crystal, PhD, director of the Rutgers Center for Health Services Research.
“Policies also need to be attentive to the possibility that, if not well managed, reductions in access to prescribed opioids could lead some individuals with pain conditions and other complications, including OUD, to turn to heroin and other illicit drugs, in an increasingly dangerous environment.”
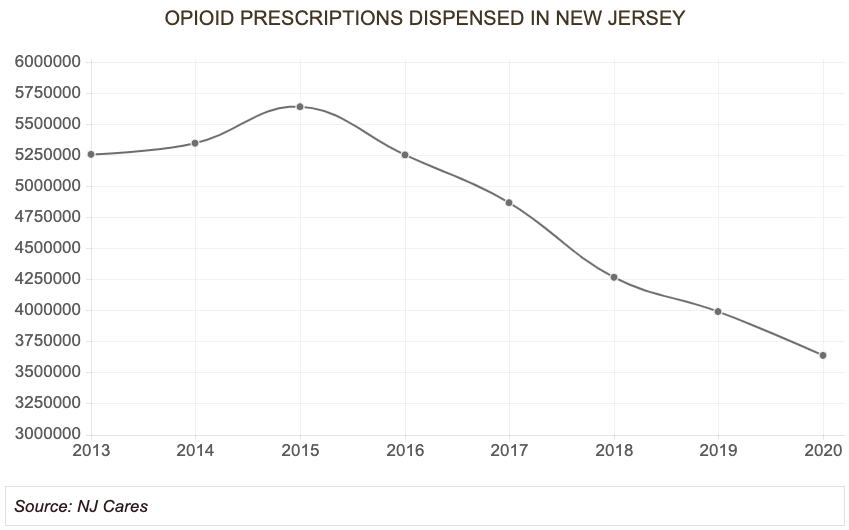
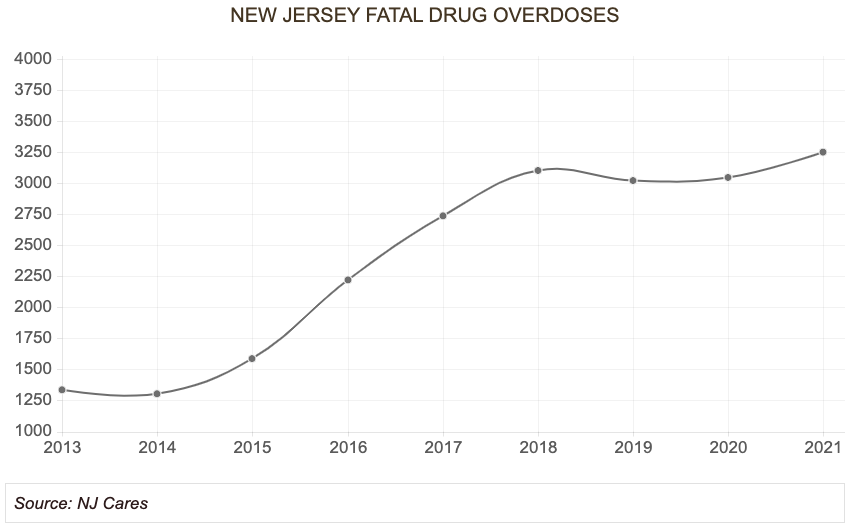
Since their peak in 2015, when over 5,640,000 opioid prescriptions were filled in New Jersey, opioid prescribing has fallen over 35% in the state. That coincided with an alarming increase in overdose deaths as illcit fentanyl began to flood New Jersey.
Comorbid Conditions
Rutgers researchers say more attention needs to be paid to people who survive overdoses, who often live with multiple health problems and comorbid conditions. In 2019, over half suffered from major depression (51%), while others had alcohol use disorder (39%), hepatitis C (30%), bipolar disorder (28%), cannabis use disorder (26.5%) sedative/hypnotic use disorder (21%) or schizophrenia (11.5%).
Notably, less than a third (30.4%) of New Jersey’s overdose survivors were diagnosed with a chronic pain condition, suggesting the state’s focus on limiting pain medication was misdirected at a time when more resources were needed throughout the state’s healthcare system, particularly for mental health.
“The high level of behavioral health and medical comorbidity that we identified among individuals with overdoses has important implications for interventions in a system in which substance use treatment, mental health care, and primary medical care are often siloed,” Crystal and his colleagues wrote.
“Interventions for conditions such as alcohol use disorder, sedative-hypnotic use disorder, and chronic obstructive pulmonary disease could reduce overdose risk. High rates of mental health comorbidity among this population, including major depression, bipolar disorder and schizophrenia, also highlight the need for concomitant mental health treatment.”
New Jersey is not alone in its failed attempt to end the overdose crisis. As PNN has reported, nearly two dozen states have implemented laws limiting the initial supply of opioid medication; 17 states limit prescriptions to 7 days supply, two states cap them at 5 days, and four states limit prescriptions to just 3 days.
These and other efforts to reduce opioid use, such as prescription drug monitoring programs (PDMPs), have resulted in prescription opioid use falling to 20-year lows in the United States, even while overdose deaths surged to record highs. Over 93,000 Americans died of drug overdoses in 2020, with the vast majority linked to illicit fentanyl and other street drugs.
The trend continues in New Jersey. In the first six months of 2021, the state reported 1,626 fatal overdoses, nearly three dozen more deaths than were recorded during the same period last year. New Jersey is on track to have a record 3,250 fatal overdoses by the end of the year.
